What is HAN? HAN is the delivery of artificial nutrition at home! Historically PN was only a hospital treatment but thanks to innovation it’s now given to those in need at home. Without this essential homecare a lot of people would be doomed to live in a hospital or some sort of care facility or just be left in a state of malnutrition and decline!
My journey to needing PN. I lived
normally for the first 55 years of my life; I was generally fighting fit, working and bringing up the children. During the late spring into summer 2015 I realised something was not right with my stomach and digestion. I had the odd stomach ache as well as the need to rush to the loo up to 12 times a day, all in all it was pretty horrible. Unsure if it was a temporary problem I waited to see if it would pass - which it didn’t - so I gave in and went to see my GP in August 2015. This was the start of the hardest and most unsettling part of my five-year journey.
As the wheels of the NHS turned slowly, it was a stop-start process having every test and scan under the sun and what turned out to be the wrong diagnosis mid-way through September 2016; small intestine bacterial overgrowth (SIBO). I was put on a low FODMAPS diet. I followed the diet for at least nine months, sadly there was no let up in symptoms but I stuck with it. If anything I got worse and the weight was falling off and my energy levels fluctuated. My former healthy weight was eight and a half stone, it went down to six stone, a lot to lose.
So, what was the point that I decided enough was enough? The easy answer to this is that my body decided for me. One weekend in June 2017 I was due to go out with my walking group for our usual five miles outing somewhere scenic; I woke up knowing I couldn’t get out of bed let alone go for a walk. I had a new excruciating
pain throughout my stomach. It recurred during the following month until a friend urged me to go back to my GP. It took someone who didn’t see me frequently to realise I needed to take decisive action. My GP arranged admission to the hospital which was to become my home from early July until the end of October.
As an in-patient on the Gastro ward, I was looked after by a very caring team of nurses who really took the time to get to know me. More and varied tests were performed - some quite invasive and uncomfortable. I was trialled with a naso-gastric feeding tube initially, which didn’t work as I still struggled to gain weight. It was a bit of a waiting game.
In late August I found out what was actually wrong with me, it was such a relief to be told I had chronic intestinal pseudo obstruction (CIPO), and relieved to be told it was not my fault! I had always eaten what I felt to be a normal, healthy, varied diet and I had a healthy appetite prior to 2015.
But what now? I asked about an operation or treatment - was there any potential for a cure? Then it was time to face facts, get real and talk through how my life would look from here onwards. I have a chronic disease and there is no op or cure, however, there is treatment which would, with time, get me back to some sort of more normal life – which was a goodish outcome.
So enter PN. I had a catheter inserted into a major vein on my right-hand chest wall. The PN is infused directly into my blood steam so my essential nutrition bypasses my intestines. I have been taught step by step procedures that allow me to connect and disconnect from my PN. I use an ambulatory feeding pump which goes into a rucksack so I can walk around with it. I have my PN overnight for 12 hours. The kit is heavy so the less I carry it around the better. My connection time coincides with my ‘me’ time when all I am doing is having supper - thankfully I can eat - and a bit of TV or similar restful or sedentary activity before bed.
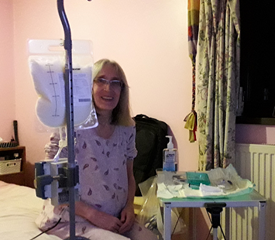
When the PN was started in hospital it was monitored and the staff did all the necessary connections and disconnections. The homecare process was explained to me. There would be a homecare company who would provide all the necessary equipment and feeds along with nurses to train me to look after it all myself. When I first went home I was still gaining weight slowly and had low energy levels. Thankfully due to not needing to attempt to keep eating the pain had gone. I enjoyed the little tastes of food I did have.
The PN started to work its magic, I was gradually putting on weight and I was keen to be trained to do my own procedures. I qualified within two to three weeks; now I could do it in my sleep – although I wouldn’t of course! The key is to follow all I was taught and to sanitise, sanitise and sanitise again. There are lots of bits and pieces to fiddle with but once you are practiced in laying it all out on the trolley provided it takes about ten minutes to disconnect and about 20 minutes to connect my PN.
How have I coped? When I was told I needed PN the nearest thing to it that I was aware of was seeing people on drips on TV shows - it was a lot for me to take in. It sounded alien, risky and plain scary but it was my only option. It’s been a lifesaver for me in every sense of the word. I have my life back. I’ve gained weight and my energetic mojo is back! I started my part-time home-based freelance translation service again. I know my limits. Being able to support myself was a concern but with my part-time work and the benefits I am entitled to that worry has been alleviated.
I’ve been tremendously thankful for the support of my family and friends. They have mainly been interested and fascinated to hear all about it - though one or two did not want me to show them my central line. Now they all understand how I’m sometimes restricted to the house at certain times and need to organise my diary around the hook-up timings on the days I am feeding (which is now only three nights a week as I have made good progress over the last year). In fact the doctors don’t want me to put on any more weight now!
Good news! I now find I can eat substantially again but I have to be careful with my oral diet to avoid the bathroom problems - and while this symptom is still with me it is a lot more in my control – for example, no more onion bhajis with an Indian, and I eat white bread ‘as it’s good for my health’ when everyone else is told to eat wholemeal!
What about the future? I hope to carry on doing what I am, living my life again in a lot of ways quite normally with the help of my PN and the hospital team who support me. Since my recent big ‘60th’ birthday, I am more an ‘autumn chicken’ so to speak and no doubt other aspects of becoming older will start to take effect but until then I want to make the most of the health PN has given me back from where I was three and even five years ago.
Hope for the future? I guess research and innovation in the medical world will seek to help those with strange stomach and bowel diseases. In the meantime I am glad I have PN, together with the support of my family, friends and my nutrition team combined with PINNT, a lovely bunch of people who are there for each other, I remain thankful for the progress I have made. I look forward to the time when we can meet in-person once again.